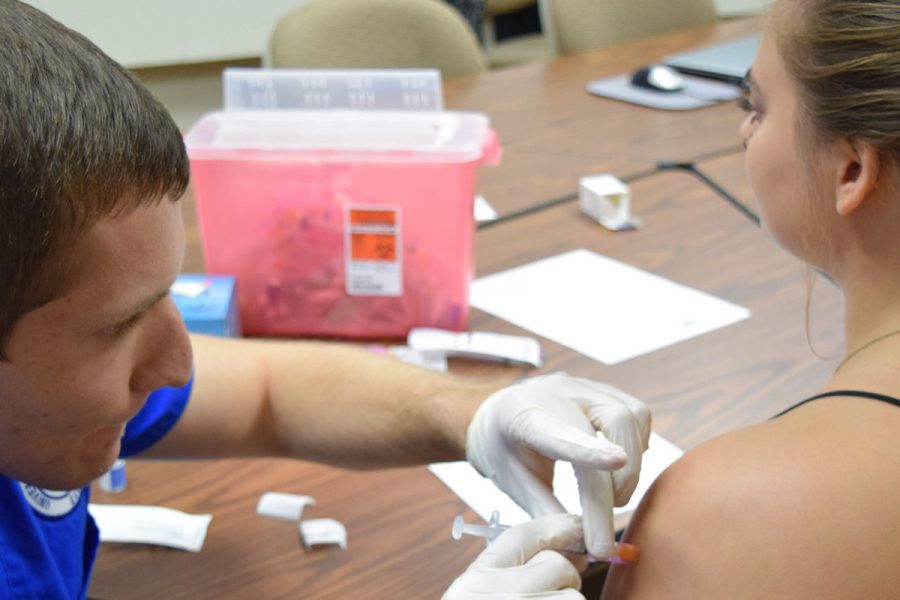
Shortage of registered nurses projected to grow into the next decade
Studies look at the causes of the deficit and plan for the future
More stories from Deanna Kolell
In an uncertain economy and job market, nursing remains a field constantly in demand.
According to the Bureau of Labor Statistics’ Employment Projections for 2012-22, the registered nursing workforce is expected to grow to almost 1.1 million by 2022, including new and replacement jobs.
Although enrollment in nursing programs has been increasing across the country, experts project massive shortages in the coming years. In an article from Health Affairs, the researchers concluded the workforce would be short 260,000 registered nurses by 2025.
This is an issue with effects at a national, state and local level. Steven Ackerson, a non-traditional third-year nursing student, said nursing faculty taught them early on about the climate they will face in the workforce because of nursing shortages.
“The nursing shortage is a complex and multifaceted issue that has no silver bullet solution,” Ackerson said. “We may think that the scope of the problem puts it beyond us. There are steps that I think all of us can take toward combating the problem.”
The first step in combating the problem is identifying the main issues contributing to nursing shortages.
Shortage of nursing school faculty is restricting nursing program enrollments
Nursing professor Katherine Sell said although the undergraduate nursing program is experiencing a steady growth in enrollment, the inadequate pool of nursing faculty limits the number of students they can accept.
As the result of budget cuts, remaining nursing staff had to increase their individual workloads by 25 students for two years. Despite this, the program must still turn students away.
“Without additional faculty and instructors, we are unable to admit more students into the program,” Sell said. “There is also a limit to the number of students that our area healthcare agencies can accommodate in various clinical agencies.”
Ackerson agreed with this assessment, warning until the state provides adequate funding for the resources nursing programs need, the projected shortage will be difficult to reduce.
At a national level, the American Association of Colleges of Nursing (AACN) reported US nursing programs turned away 79,659 qualified applicants in 2012, not only because of limited faculty, but also in response to limited classroom space, clinical sites and budget cuts.
A significant segment of nursing workforce is nearing retirement age
The Health Resources and Services Administration projected in 10-15 years, more than 1 million registered nurses will reach retirement age, around one-third of the workforce.
In addition, The Atlantic projected around 700,000 nurses will retire or leave the labor force by 2024.
Sell said it is important to have a balanced mix of experienced staff working with less seasoned nurses, however, nurses are leaving the workforce faster than new trainees can fill the vacancies.
The “Baby Boomer” generation is in greater need of healthcare
Today, there are more citizens aged 65 and older than there ever has been at any time in United States history. According to The Atlantic, there will be 69 million senior citizens by 2030 and 88.5 million by 2050.
Ackerman said this is significant because the Affordable Care Act has expanded health insurance coverage to include millions of Americans and senior citizens who often have two or more chronic diseases, increasing their need for healthcare.
Insufficient staffing can lead to stress, burnout and low quality of care
A shortage of nurses on staff can lead to overwork and burnout, which can put nurses at risk for making errors.
Lower nurse staffing levels have also been associated with increased patient mortality rates and lower quality of care, while higher nurse staffing levels are associated with fewer deaths, lower rates of infection and shorter hospital stays.
Kathy Hastreiter, a 2015 Eau Claire nursing alumna, is now working at Columbia St. Mary’s-Ozaukee in the Intensive Care Unit/Acuity Adaptable Unit. She said she has experienced a shortage of staff in her unit before.
“I know that burnout is a huge issue, particularly in ICUs,” Hastreiter said. “Nurses are often viewed as overworked and underpaid.”
Planning for the future
A long-term strategy to combat nursing shortages, as prescribed by The Atlantic, is opening paths to earning a degree.
Eau Claire is working toward that same goal by participating in the BSN@Home program, which began in 2013. Partnered with five other universities from the UW-System, this online program allows people flexibility in earning a nursing degree.
Hastreiter called for additional action, such as discussing how nurses can go back to school, working on preventing workplace injuries and creating a team-oriented environment to prevent burnout.
Finally, Ackerson suggested advocating for reasonable education budget levels, promoting nursing as a career to youths and petitioning lawmakers to establish safe nurse staffing levels.
Although he said there is no quick solution to the nursing shortages, Ackerman said he looks forward to his challenging and rewarding future as a nurse.
“The present and future nursing climate offers tremendous opportunities for professional growth with the potential to develop a competitive and diverse nursing practice,” Ackerman said. “As nurses, we will continually be challenged…to develop new, creative and inventive ways to provide care more efficiently while maintaining high quality.”
To learn more about projected nursing shortages, causes and solutions, visit the American Association of Colleges of Nursing website.